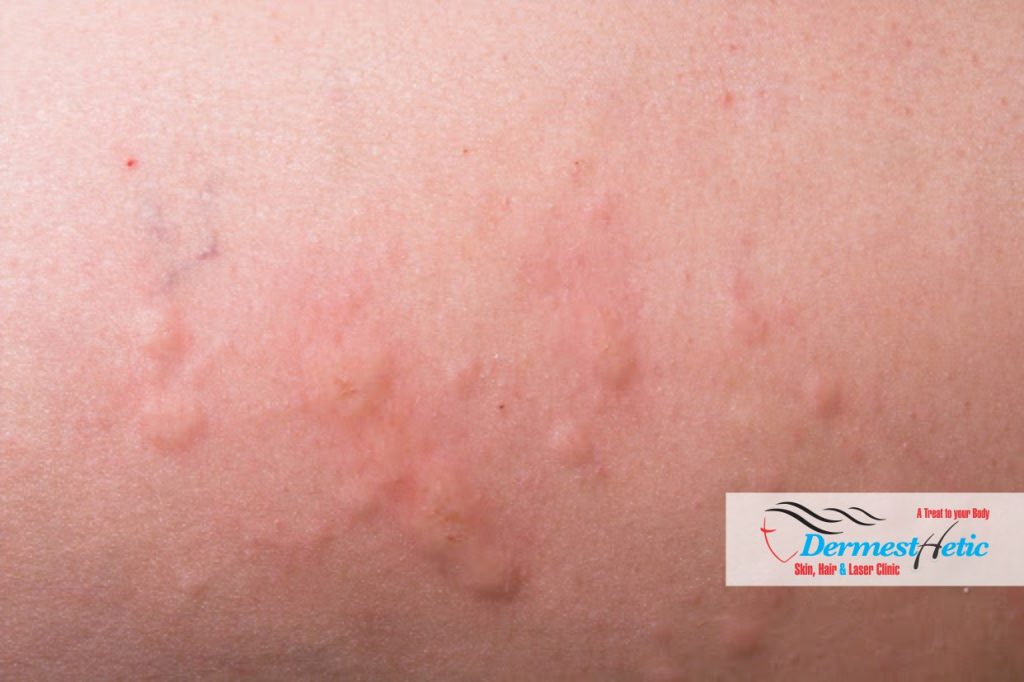
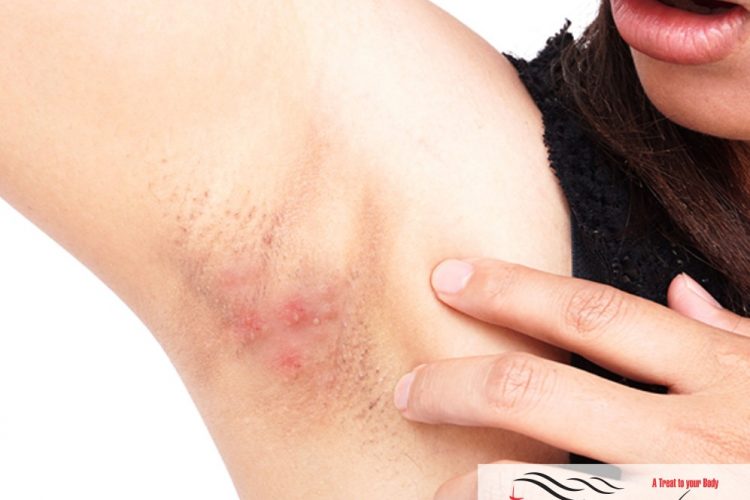
Hidradenitis Suppurativa (HS) also known as acne inversa is a skin disease that usually begins as pimples in the armpits (usually both armpits) or in the groin (pubic area). It is a condition that causes painful bumps under your skin in the hair roots near some of your sweat glands. The bumps can get infected. When that happens, pockets form under your skin and fill with pus. They can smell bad when they break open. These pimples are unique in a way that they tend to develop in places that everyday pimples do not appear i.e., everyday pimples appear on the face and chest/back, the condition mostly affects areas where the skin rubs together, such as the armpits, groin, buttocks and breasts. Hidradenitis suppurativa pimples later on turn into deep boils which rupture and gives rise to pus filled cysts or boils that do not heal and keep on recurring for months to years. We at DERMESTHETIC Silakot & Lahore, Pakistan have experienced dermatologists and cosmetologists diagnosing and curing these diseases.
Consultation
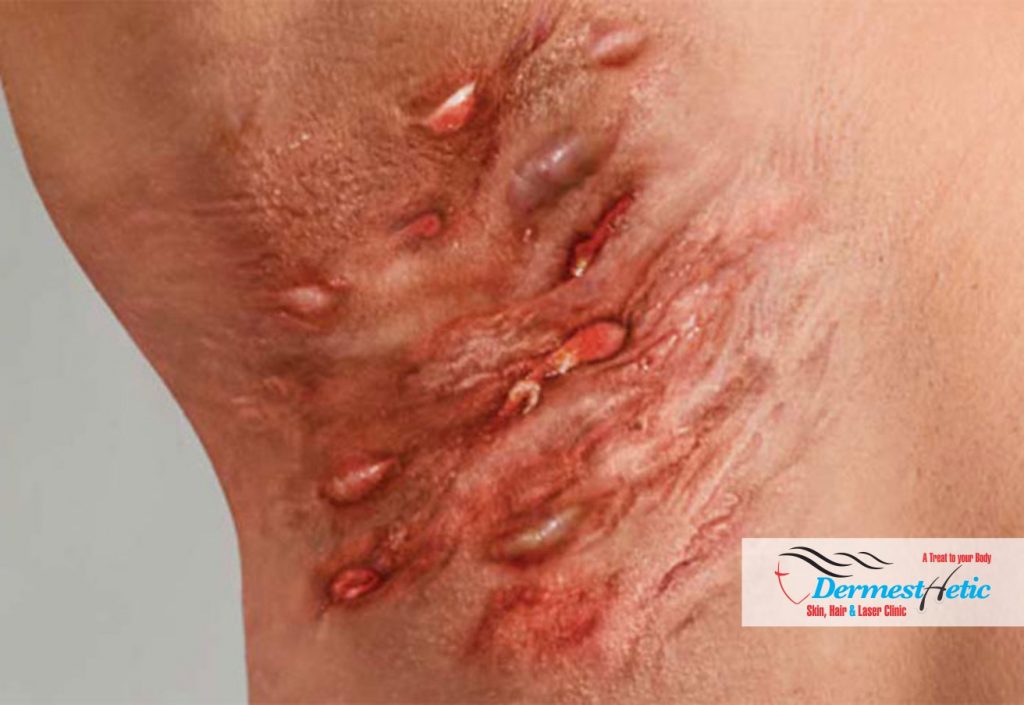
At DERMESTHETIC Silakot & Lahore, Pakistan we are committed to providing patients with the most advanced and authentic treatment of Hidradenitis suppurativa Lahore & Sialkot in Pakistan. Hidradenitis suppurativa causes considerable pain, discomfort and agony to most patients. HS (Hidradenitis Suppurativa) is a difficult disease to treat, we at DERMESTHETIC are the experts and specialists to treat Hidradenitis Suppurative and receive cases from all over Pakistan. If you are suffering from this frustrating condition, you are not alone. Here at DERMESTHETIC our hidradenitis suppurativa specialists can assure your well-being, each one is well versed in treating all types of hidradenitis, from mild to very severe. We at DERMESTHETIC have hundreds of satisfied patients successfully treated with our latest treatment techniques including medications, lasers etc.
Hidradenitis suppurativa is characterized clinically by:
- Open double-headed comedones;
- Painful firm papules and nodules;
- Pustules, fluctuant pseudocysts, and abscesses;
- Draining sinuses linking inflammatory lesions;
- Hypertrophic and atrophic scars.
Hidradenitis suppurativa often starts at puberty, is most active between the ages of 20 and 40 years, and in women can resolve at menopause. It is three times more common in females than in males. Associations and risk factors include:
- Other family members with hidradenitis suppurativa; 30–40% report at least one other family member affected
- Obesity and insulin resistance (metabolic syndrome)
- Cigarette smoking
- African ethnicity
- Follicular occlusion syndrome: acne conglobata, dissecting cellulitis, pilonidal sinus
- Inflammatory bowel disease, particularly Crohn disease
- Other skin disorders: psoriasis, acne, hirsutism
- Comorbidities: hypertension, diabetes mellitus, dyslipidaemia, thyroid disorders, arthropathies, polycystic ovary syndrome, adverse cardiovascular outcomes
- Drugs: lithium, sirolimus, biologics
- Syndromes
- PAPA syndrome
- PASH syndrome (pyoderma gangrenosum, acne, suppurative hidradenitis)
- PAPASH syndrome (pyogenic arthritis, pyoderma gangrenosum, acne, suppurative hidradenitis).
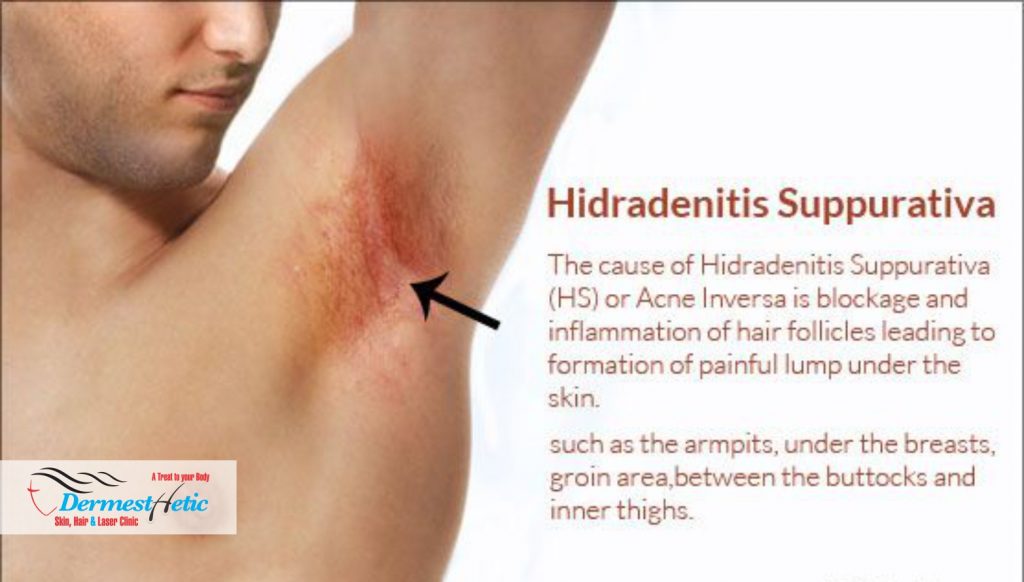
We at DERMESTHETIC have such expertise and knowledge and you may meet with our doctors who are rated as the BEST SKIN SPECIALISTS AND DERMATOLOGISTS IN LAHORE, PAKISTAN with special interest in ENS.
Causes of hidradenitis suppurativa
The exact cause of hidradenitis suppurativa isn’t known. It develops when hair follicles in the skin become blocked. Experts think it could be connected to hormones, inherited genes and immune system problems. Smoking, excess weight and metabolic syndrome also might play a role.
Although ‘hidradenitis’ implies an inflammatory disorder of sweat glands, we now know hidradenitis suppurativa is an autoinflammatory syndrome. The exact pathogenesis is not yet understood. Factors involved in the development of hidradenitis suppurativa include:
- Follicular occlusion
- An abnormal cutaneous or follicular microbiome
- Release of pro-inflammatory cytokines
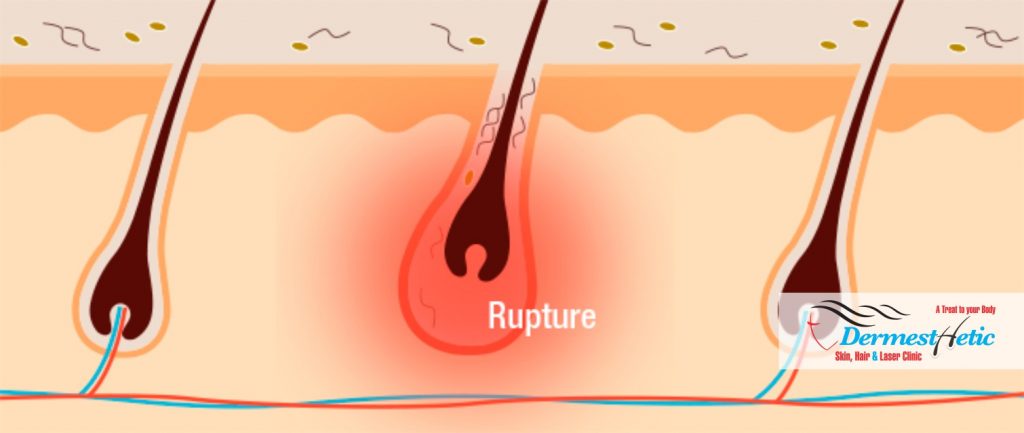
- Inflammation causing rupture of the follicular wall, destroying sebaceous and apocrine glands and ducts.
Symptoms of hidradenitis suppurativa
Hidradenitis suppurativa tends to start after puberty. It can persist for many years and worsen over time, with serious effects on your daily life and emotional well-being. Medications and surgery can help manage symptoms and prevent complications.
Hidradenitis suppurativa can affect one spot or multiple areas of the body. Signs and symptoms of the condition include:
- Blackheads. Small pitted areas of skin containing blackheads — often appearing in pairs or a “double-barreled” pattern — are a common feature.
- Painful pea-sized lumps. The condition usually starts with a single, painful lump under the skin that persists for weeks or months. Later more bumps form. They usually appear in areas with hair follicles with many oil and sweat glands, such as the armpits, groin and anal area. They also occur where skin rubs together, such as the inner thighs, breast and buttocks.
- Tunnels. Over time, tracts connecting the lumps may form under the skin. These wounds heal very slowly, if at all, and can leak pus, which may have an odor.
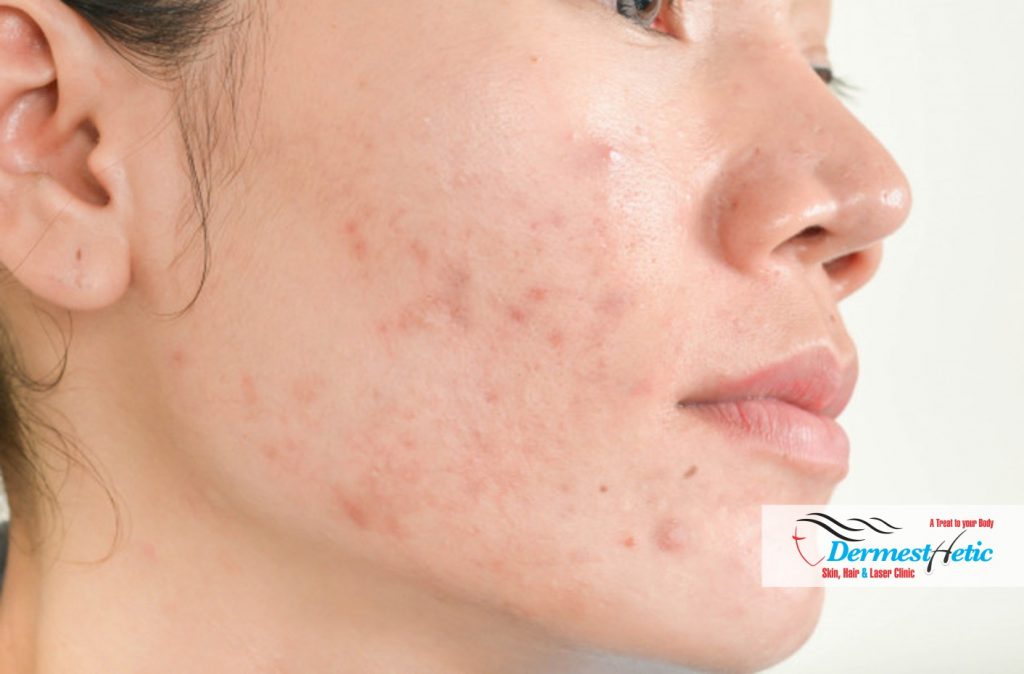
We at DERMESTHETIC at Sialkot & Lahore, Pakistan has highly qualified Dermatologists/Cosmetologists who are expert in Hidradenitis suppurativa (HS) treatments and procedures. Some people with this condition experience only mild symptoms. Excess weight, stress, hormonal changes, heat or humidity may worsen symptoms. In women, the disease severity may lessen after menopause. And don’t forget, waiting for HS to clear on its own can be frustrating. Without treatment, HS can cause low self-esteem, depression and anxiety. To avoid these possible outcomes, dermatologists recommend that people treat hidradenitis suppurativa at an earliest stage as treatment may prevent new breakouts.
Types of hidradenitis suppurativa
Regular HS: Its most common form. Recurrent inflammatory lesions in typical locations for at least 6 months;
Frictional furuncle: Regular HS plus multiple deep nodules and abcesses on sites exposed to enhanced friction (abdomen, thighs, buttocks);
Scarring folliculitis: Regular HS plus pustules, cysts, superficial nodules, depressed cribriform scarring, and double-headed comedones.
Conglobata: Cyst formation and acne conglobata lesions on the back and face;
Syndromic: HS in conjunction with syndromic features (PAPA, PASH, PAPASH).
Surgical and other procedural measures:
- Incision and drainage of acute abscesses
- Local excision of persistent nodules, abscesses, and sinuses
- Deroofing and curettage of persistent abscesses and sinuses
- Radical excisional surgery of an entire affected area
- Laser ablation (CO2) of nodules, abscesses, and sinuses
- Laser/light hair removal.
Treatment of hidradenitis suppurativa
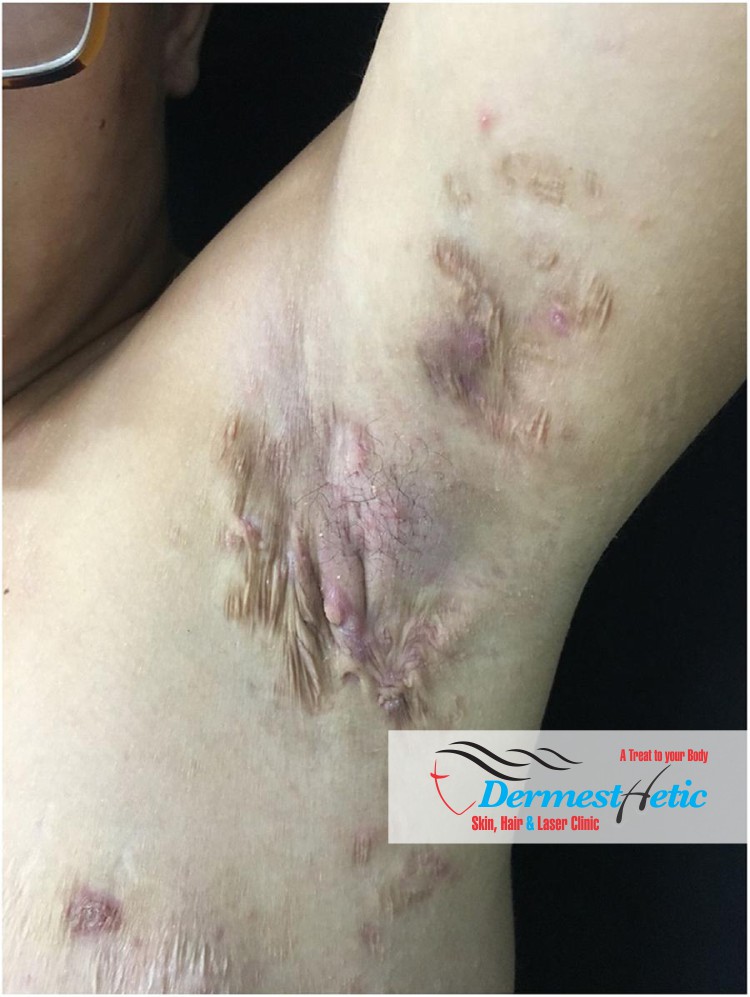
We at DERMESTHETIC at Sialkot & Lahore, Pakistan have experienced dermatologists and cosmetologists treating the hidradenitis suppurativa (HS) and properly advise the patient regarding the treatment after making proper diagnosis. Treatment options for moderate to severe disease include oral antibiotics with immunomodulatory properties such as tetracycline (where available), doxycycline, clindamycin and rifampin; antiandrogenic therapies; systemic immunosuppressive therapy, including tumor necrosis factor (TNF) inhibitors and laser.
How is hidradenitis suppurativa treated?
- Sit in a warm bath and/or apply warm compresses to the affected area for 10 minutes at a time.
- Apply topical cleansing agents, including antibacterial soaps, antiseptics, and acne washes to reduce/kill bacteria.
- Warm compress. A warm compress can immediately reduce pain in the affected area. …
- Turmeric has strong anti-inflammatory, antimicrobial, and antibacterial properties.
- Honey.
- Tea tree oil.
- Aloe vera.
- Rubbing alcohol.
- Zinc.
- Neem oil.
Side effects
Persistent and severe hidradenitis suppurativa often causes complications, including:
- Infection. The affected area is susceptible to infection.
- Scars and skin changes. The wounds may heal but leave rope-like scars or pitted skin.
- Restricted movement. Sores and scar tissue may cause limited or painful movement, especially when the disease affects the armpits or thighs.
- Obstructed lymph drainage. The most common sites for hidradenitis suppurativa also contain many lymph nodes. Scar tissue can interfere with the lymph drainage system, which may result in swelling in the arms, legs or genitals.
- Social isolation. The location, drainage and odor of the sores can cause embarrassment and reluctance to go out in public, leading to sadness or depression.