Dermatitis also known as eczema, is a group of diseases that results in itching or/and inflammation of the skin. Dermatitis (eczema) is a condition that makes your skin red and itchy. It’s common in children but can occur at any age. Some types of Eczema are long lasting (chronic) and tends to flare periodically. These diseases are characterized by itchiness, red skin and a rash. In cases of short duration, there may be small blisters, while in long-term cases the skin may become thickened. The area of skin involved can vary from small to the entire body. It may be accompanied by asthma or hay fever. Healthy skin helps retain moisture and protects you from bacteria, irritants and allergens. Eczema is related to a gene variation that affects the skin’s ability to provide this protection. This allows your skin to be affected by environmental factors, irritants and allergens. Sometimes your dermatologist will combine treatments to get the best results and to avoid developing drug-resistant bacteria. Treatment could include lotions or gels you put on blemishes or sometimes entire areas of skin, such as the chest or back (topical medicines). You might also take medicines by mouth (oral medicines). If you want to treat eczema, you should see a dermatologist. We at DERMESTHETIC at Sialkot & Lahore, Pakistan have experienced dermatologists and cosmetologists diagnosing and curing these diseases.
Types of Eczema/Dermatitis
 Dermatitis is a group of skin conditions that includes (1) atopic dermatitis, (2) allergic contact dermatitis, (3) irritant contact dermatitis, (4) Perioral dermatitis, (5) seborrheic eczema, (6) phototoxic dermatitis and (6) stasis dermatitis. The exact cause of dermatitis is often unclear. Cases may involve a combination of irritation, allergy and poor venous return The type of dermatitis is generally determined by the person’s history and the location of the rash. For example, irritant dermatitis often occurs on the hands of people who frequently get them wet. Allergic contact dermatitis occurs upon exposure to an allergen, causing a hypersensitivity reaction in the skin.
Dermatitis is a group of skin conditions that includes (1) atopic dermatitis, (2) allergic contact dermatitis, (3) irritant contact dermatitis, (4) Perioral dermatitis, (5) seborrheic eczema, (6) phototoxic dermatitis and (6) stasis dermatitis. The exact cause of dermatitis is often unclear. Cases may involve a combination of irritation, allergy and poor venous return The type of dermatitis is generally determined by the person’s history and the location of the rash. For example, irritant dermatitis often occurs on the hands of people who frequently get them wet. Allergic contact dermatitis occurs upon exposure to an allergen, causing a hypersensitivity reaction in the skin.
Less common types of Eczema/Dermatitis
Dyshidrosis (dyshidrotic eczema, pompholyx, vesicular palmoplantar dermatitis) only occurs on palms, soles, and sides of fingers and toes. Tiny opaque bumps called vesicles, thickening, and cracks are accompanied by itching, which gets worse at night. A common type of hand eczema, it worsens in warm weather.
Discoid eczema (nummular eczema, exudative eczema, microbial eczema) is characterized by round spots of oozing or dry rash, with clear boundaries, often on lower legs. It is usually worse in winter. Cause is unknown, and the condition tends to come and go.
Venous eczema (gravitational eczema, stasis dermatitis, varicose eczema) occurs in people with impaired circulation, varicose veins, and edema, and is particularly common in the ankle area of people over 50 years. There is redness, scaling, darkening of the skin, and itching. The disorder predisposes to leg ulcers.
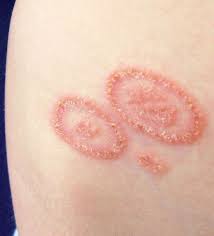 Dermatitis herpetiformis (Duhring’s disease) causes intensely itchy and typically symmetrical rash on arms, thighs, knees, and back. It is directly related to celiac disease, can often be put into remission with appropriate diet, and tends to get worse at night.
Dermatitis herpetiformis (Duhring’s disease) causes intensely itchy and typically symmetrical rash on arms, thighs, knees, and back. It is directly related to celiac disease, can often be put into remission with appropriate diet, and tends to get worse at night.
Neurodermatitis (lichen simplex chronicus, localized scratch dermatitis) is an itchy area of thickened, pigmented eczema patch that results from habitual rubbing and scratching. Usually there is only one spot. Often curable through behavior modification and anti-inflammatory medication. Prurigo nodularis is a related disorder showing multiple lumps.
Autoeczematization (autosensitization) is an eczematous reaction to an infection with parasites, fungi, bacteria or viruses. It is completely curable with the clearance of the original infection that caused it. The appearance varies depending on the cause. It always occurs some distance away from the original infection.
Viral-There are eczemas overlaid by viral infections (eczema herpeticum or vaccinatum), and eczemas resulting from underlying disease (e.g., lymphoma). Eczemas originating from ingestion of medications, foods, and chemicals, have not yet been clearly systematized. Other rare eczematous disorders exist in addition to those listed here.
Consultation
No lab test is needed to identify atopic dermatitis (eczema). Your doctor preferably a dermatologist will likely make a diagnosis by examining your skin and reviewing your medical history. He or she may also use patch testing or other tests to rule out other skin diseases or identify conditions that accompany your eczema. Doctors don’t know exactly what causes eczema. Diagnosis of eczema is based mostly on the history and physical examination. In uncertain cases, skin biopsy may be useful. Those with eczema may be especially prone to misdiagnosis of food allergies. Patch tests are used in the diagnosis of allergic contact dermatitis.
The most common type of eczema, atopic dermatitis, resembles an allergy. But the skin irritation, which is more often seen in children rather than adults, is not an allergic reaction. No cure has been found for atopic dermatitis. But treatments and self-care measures can relieve itching and prevent new outbreaks. For example, it helps to avoid harsh soaps, moisturize your skin regularly, and apply medicated creams or ointments. Before starting treatment, a dermatologist diagnosis the type of eczema. We at DERMESTHETIC at Sialkot & Lahore, Pakistan have such expertise and knowledge.
Causes
The current thinking is that eczema is caused by a combination of factors that include:
- Genetics
- Abnormal function of the immune system
- Environment
- Activities that may cause skin to be more sensitive
- Defects in the skin barrier that allow moisture out and germs in.
Eczema Symptoms
 We at DERMESTHETIC at Sialkot, Lahore, Pakistan have experienced dermatologists treating the dermatitis/eczema along with counselling on psychological issue which may crop up due to dermatitis/eczema and properly advise the patients regarding the treatment. Dermatitis symptoms vary with all different forms of the condition. They range from skin rashes to bumpy rashes or including blisters. Although every type of dermatitis has different symptoms, there are certain signs that are common for all of them, including redness of the skin, swelling, itching and skin lesions with sometimes oozing and scarring. Although the symptoms of atopic dermatitis vary from person to person, the most common symptoms are dry, itchy, red skin. Perioral dermatitis refers to a red bumpy rash around the mouth. Atopic dermatitis (eczema) signs and symptoms vary widely from person to person and include:
We at DERMESTHETIC at Sialkot, Lahore, Pakistan have experienced dermatologists treating the dermatitis/eczema along with counselling on psychological issue which may crop up due to dermatitis/eczema and properly advise the patients regarding the treatment. Dermatitis symptoms vary with all different forms of the condition. They range from skin rashes to bumpy rashes or including blisters. Although every type of dermatitis has different symptoms, there are certain signs that are common for all of them, including redness of the skin, swelling, itching and skin lesions with sometimes oozing and scarring. Although the symptoms of atopic dermatitis vary from person to person, the most common symptoms are dry, itchy, red skin. Perioral dermatitis refers to a red bumpy rash around the mouth. Atopic dermatitis (eczema) signs and symptoms vary widely from person to person and include:
- Dry skin;
- Itching, which may be severe, especially at night;
- Red to brownish-gray patches, especially on the hands, feet, ankles, wrists, neck, upper chest, eyelids, inside the bend of the elbows and knees, and in infants, the face and scalp;
- Small, raised bumps, which may leak fluid and crust over when scratched;
- Thickened, cracked, scaly skin;
- Raw, sensitive, swollen skin from scratching;
Atopic dermatitis most often begins before age 5 and may persist into adolescence and adulthood. For some people, it flares periodically and then clears up for a time, even for several years. Although the location may vary, the primary symptom of this condition is itchy skin. More rarely, it may appear on the genital area, such as the vulva or scrotum.
Treatments
 We at DERMESTHETIC at Silakot & Lahore, Pakistan have experienced dermatologists and therapists treating the dermatitis/eczema and properly advise the patient regarding the treatment after making diagnosis of the type of dermatitis/eczema. Treatment of dermatitis/eczema depends on whether inflammation or infection are present. Treatment of dermatitis/eczema is typically with moisturizers and steroid creams. The steroid creams should generally be of mid- to high strength and used for less than two weeks at a time as side effects can occur. Antibiotics may be required if there are signs of skin infection. Contact dermatitis is typically treated by avoiding the allergen or irritant. Antihistamines may help with sleep and to decrease nighttime scratching.
We at DERMESTHETIC at Silakot & Lahore, Pakistan have experienced dermatologists and therapists treating the dermatitis/eczema and properly advise the patient regarding the treatment after making diagnosis of the type of dermatitis/eczema. Treatment of dermatitis/eczema depends on whether inflammation or infection are present. Treatment of dermatitis/eczema is typically with moisturizers and steroid creams. The steroid creams should generally be of mid- to high strength and used for less than two weeks at a time as side effects can occur. Antibiotics may be required if there are signs of skin infection. Contact dermatitis is typically treated by avoiding the allergen or irritant. Antihistamines may help with sleep and to decrease nighttime scratching.
The most common types of medicines and therapies that doctors use to treat dermatitis/eczema include:
Lifestyle – Bathing once or more a day is recommended, usually for five to ten minutes in warm water. Soaps should be avoided as they tend to strip the skin of natural oils and lead to excessive dryness. People can wear clothing designed to manage the itching, scratching and peeling.
Moisturizers – Low-quality evidence indicates that moisturizing agents (emollients) may reduce eczema severity and lead to fewer flares. Some emollients may reduce the number of flares in people with dermatitis. In children, oil-based formulations appear to be better and water-based formulations are not recommended. It is unclear if moisturizers that contain ceramides are more or less effective than others. Products that contain dyes, perfumes or peanuts should not be used. Occlusive dressings at night may be useful. Some moisturizers or barrier creams may reduce irritation in occupational irritant hand dermatitis, a skin disease that can affect people in jobs that regularly come into contact with water, detergents, chemicals or other irritants.
Antihistamine – There is little evidence for antihistamine; they are thus not generally recommended. Sedative antihistamines such as diphenhydramine may be tried in those who are unable to sleep due to eczema.
Colloidal Oatmeal – Oatmeal contains avenanthramide (anthranilic acid amides), which can have an anti-inflammatory effect.
Corticosteroids – For more-severe cases, your doctor may prescribe oral corticosteroids, such as prednisone. These drugs are effective but can’t be used long term because of potential serious side effects. If symptoms are well controlled with moisturizers, steroids may only be required when flares occur. Corticosteroids are effective in controlling and suppressing symptoms in most cases. Once daily use is generally enough. For mild-moderate eczema a weak steroid may be used (e.g., hydrocortisone), while in more severe cases a higher-potency steroid (e.g., clobetasol propionate) may be used. In severe cases, oral or injectable corticosteroids may be used. While these usually bring about rapid improvements, they have greater side effects. Long term use of topical steroids may result in skin atrophy, stria, telangiectasia. Their use on delicate skin (face or groin) is therefore typically with caution. They are, however, generally well tolerated.
Antibiotic – Your dermatologist may prescribe an antibiotic cream if your skin has a bacterial infection, an open sore or cracks. He or she may recommend taking oral antibiotics for a short time to treat an infection.
ImmunosuppressantTopical immunosuppressant like pimecrolimus and tacrolimus may be better in the short term and appear equal to steroids after a year of use. Their use is reasonable in those who do not respond to or are not tolerant of steroids. Tacrolimus 0.1% has generally proved more effective than pimecrolimus, and equal in effect to mid-potency topical steroids. There is no link to increased risk of cancer from topical use of 1% pimecrolimus cream. When eczema is severe and does not respond to other forms of treatment, systemic immunosuppressants are sometimes used.
Injectable Biologic – injectable biologic (monoclonal antibody) called dupilumab (Dupixent). It is used to treat people with severe disease who do not respond well to other treatment options. This is a newer medication, so it doesn’t have a long track record in terms of how well it helps people. Studies have shown it to be safe if used as directed. It is very expensive.
Alternative Medicines – Limited evidence suggests that acupuncture may reduce itching in those affected by atopic dermatitis. There is currently no scientific evidence for the claim that sulfur treatment relieves eczema. It is unclear whether Chinese herbs help or harm. Dietary supplements are commonly used by people with eczema. Neither evening primrose oil nor borage seed oil taken orally have been shown to be effective. Both are associated with gastrointestinal upset. Probiotics do not appear to be effective. There is insufficient evidence to support the use of zinc, selenium, vitamin D, vitamin E, pyridoxine (vitamin B6), sea buckthorn oil, hempseed oil, sunflower oil, or fish oil as dietary supplements.
Bleach Bath – The American Academy of Dermatology recommends considering a bleach bath to help prevent flares. A diluted-bleach bath decreases bacteria on the skin and related infections.
Wet Dressings – An effective, intensive treatment for severe atopic dermatitis involves wrapping the affected area with topical corticosteroids and wet bandages. Sometimes this is done in a hospital for people with widespread lesions because it’s labor intensive and requires nursing expertise.
Light Therapy – Phototherapy – Heliotherapy – Light therapy using ultraviolet light has tentative support but the quality of the evidence is not very good. A number of different types of light may be used including UVA and UVB; in some forms of treatment, light sensitive chemicals such as psoralen are also used. Overexposure to ultraviolet light carries its own risks, particularly that of skin cancer.
Counseling – Talking with a dermatologist/therapist or other counselor may help people who are embarrassed or frustrated by their skin condition.
Side Effects
 Side effects of acne treatments vary depending on the method you choose and the potency of the medication. Immunosuppressants can cause significant side effects and some require regular blood tests. The most commonly used are ciclosporin, azathioprine, and methotrexate. They often improve as your body gets used to the medication. If your skin itches, burns, or peels heavily, tell your doctor.
Side effects of acne treatments vary depending on the method you choose and the potency of the medication. Immunosuppressants can cause significant side effects and some require regular blood tests. The most commonly used are ciclosporin, azathioprine, and methotrexate. They often improve as your body gets used to the medication. If your skin itches, burns, or peels heavily, tell your doctor.
The potential side effects for oral corticosteroids can be more serious if use continuously. Antibiotics can give you an upset stomach or make you dizzy and lightheaded. Overexposure to ultraviolet light during phototherapy carries its own risks, particularly that of skin cancer.







