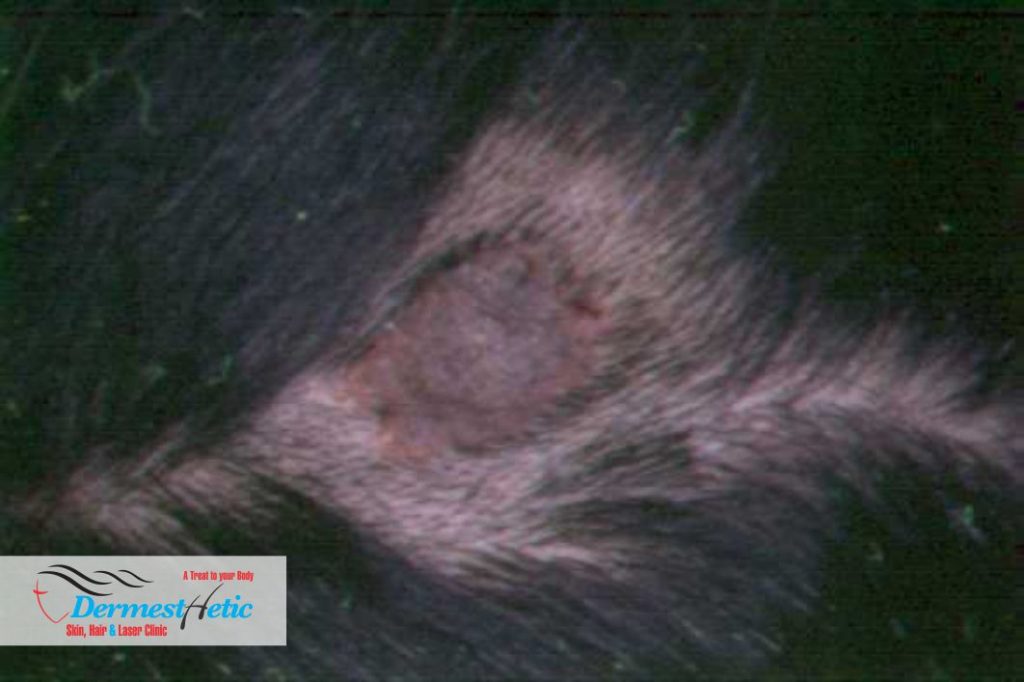
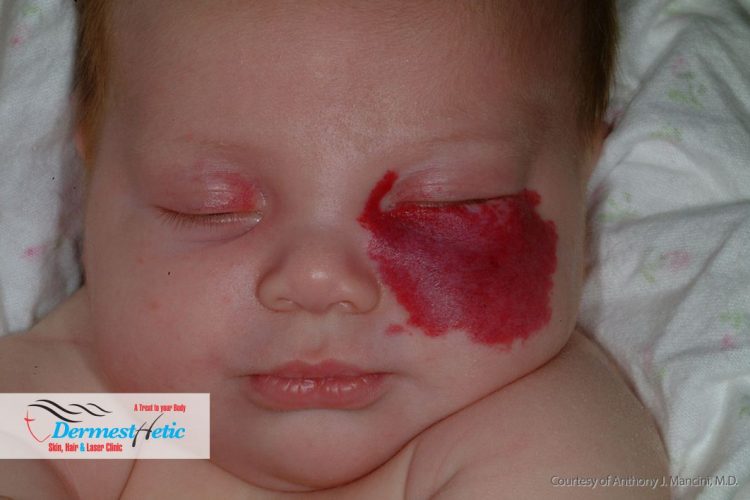
Epidermal Nevus Syndrome (ENS) also known as “Feuerstein and Mims syndrome” and “Solomon’s Syndrome is a rare disease that was first described in 1968 and consists of extensive epidermal nevi with abnormalities of the central nervous system(CNS), eyes, cardiovascular system, skeleton, genitourinary system and skin. Epidermal nevus syndromes (ENSs) are a group of rare complex disorders characterized by the presence of skin lesions known as epidermal nevi associated with additional extra-cutaneous abnormalities, most often affecting the brain, eye and skeletal systems. Epidermal nevi are overgrowths of structures and tissue of the epidermis, the outermost layer of the skin. The different types of epidermal nevi can vary in size, number, location, distribution and appearance. Neurological abnormalities that can be associated with ENSs can include seizures, cognitive impairment, developmental delays and paralysis of one side of the body. Two other terms that have been used to describe ENSs are “organoid nevus syndrome” and “keratinocytic nevus syndrome”. However, it is inappropriate to use these terms to denote a single disorder or interchangeably with epidermal nevus syndromes. Organoid nevus syndrome is a general term that could be applied to at least five different types of ENS. Keratinocytic nevus syndrome is a general term that could be applied to four different types of ENS. An epidermal nevus (plural: nevi) is an abnormal, noncancerous (benign) patch of skin caused by an overgrowth of cells in the outermost layer of skin (epidermis). Keratinocytic epidermal nevi are typically found on the torso or limbs. They can be flat, tan or brown patches of skin or raised, velvety patches. Small nevi can be removed by simple surgical excision. The nevus is cut out, and the adjacent skin stitched together leaving a small scar. Removal of a large congenital nevus, however, requires replacement of the affected skin. We at DERMESTHETIC Silakot & Lahore, Pakistan have experienced dermatologists and cosmetologists diagnosing and curing these diseases.
Consultation
At DERMESTHETIC Silakot & Lahore, Pakistan we are committed to providing patients with the most advanced and authentic treatment of CNS in Pakistan. In order to educate our patients in great detail about CNS in general, it’s causes, it’s different types and various treatment options available in the world, we provide a detailed information in this portion that the patients can educate themselves in befitting manner regarding their disease. The term “epidermal nevus syndrome” has generated significant controversy and confusion in the medical literature. Originally, the term was used to denote a disorder that was actually several different disorders erroneously grouped together. In the recent past, the term was used to denote a specific disorder now known as Schimmelpenning syndrome. However, the term epidermal nevus syndrome could be correctly applied to several different disorders. Therefore, the umbrella term “epidermal nevus syndromes” now represents a group of distinct disorders that have in common the presence of one of the various types of epidermal nevi. However, there is so far no general agreement how to classify the types of this diverse group of disorders, adding to the confusion within the medical literature.
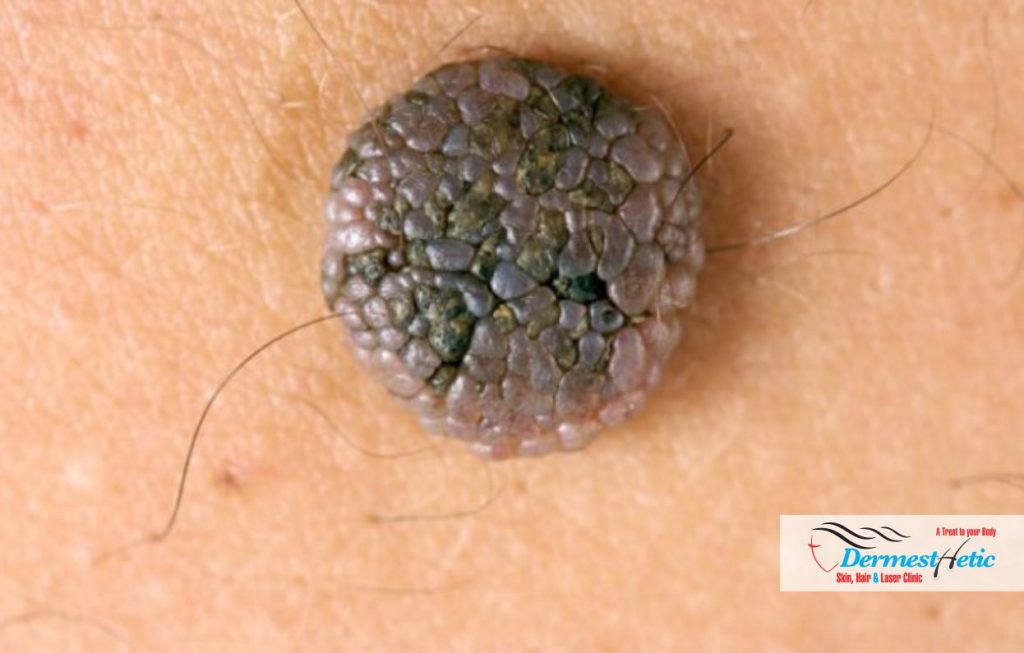
If the symptoms are unclear or if your doctor wants to confirm their suspected diagnosis, they may take a small sample of skin. This is known as a biopsy. The skin will be sent to a lab, where it’ll be examined. The examination can diagnose the type of ENS you have. It can also rule out other possible disorders or infections. Combining two or more treatments often gives the best results. Before starting treatment, a dermatologist should be consulted. We at DERMESTHETIC have such expertise and knowledge and you may meet with our doctors who are rated as the BEST SKIN SPECIALISTS AND DERMATOLOGISTS IN LAHORE, PAKISTAN with special interest in ENS.
Causes
Most epidermal nevus syndromes are thought to be caused by a gene mutation that occurs after fertilization of the embryo (postzygotic mutation), at an early stage of embryonic development. Affected individuals have some cells with a normal copy of this gene and some cells with the abnormal gene (mosaic pattern). Epidermal nevi (EN) are congenital hamartomas of embryonal ectodermal origin classified on the basis of their main component; the component may be sebaceous, apocrine, eccrine, follicular, or keratinocytic. An estimated one third of individuals with epidermal nevi have involvement of other organ systems; hence, this condition is considered to be an epidermal nevus syndrome (ENS). Solomon defines epidermal nevus syndrome as a sporadic neurocutaneous linkage of congenital ectodermal defects in the skin, brain, eyes, and/or skeleton. Epidermal nevus syndrome is often termed the Solomon syndrome. Schimmelpenning first detailed epidermal nevi with neurologic anomalies; hence, the term Schimmelpenning syndrome. The term organoid nevus may be used to emphasize the admixture of epidermal cells often evident in individual lesions of epidermal nevi.
Symptoms
Epidermal nevus syndromes encompass a wide variety of disorders. The specific symptoms present, severity and prognosis can vary greatly depending on the specific type of ENS and the presence and extent of associated extra-cutaneous symptoms. The onset and progression of these disorders varies greatly as well. Epidermal nevi have also been classified as “hamartomas”, a rather vague and ambiguous term for benign tumor-like malformations that can affect any area of the body. “Hamartomas” are composed of mature cells and tissue normally found in the affected area. There are different types of epidermal nevi based upon their main component. Epidermal nevi are usually present at birth (congenital) and appear as a patch or plaque of overgrown skin. Epidermal nevi often occur on the trunk, limbs, face or scalp. Epidermal nevi can be striking and obvious in appearance or subtle and easy to miss.
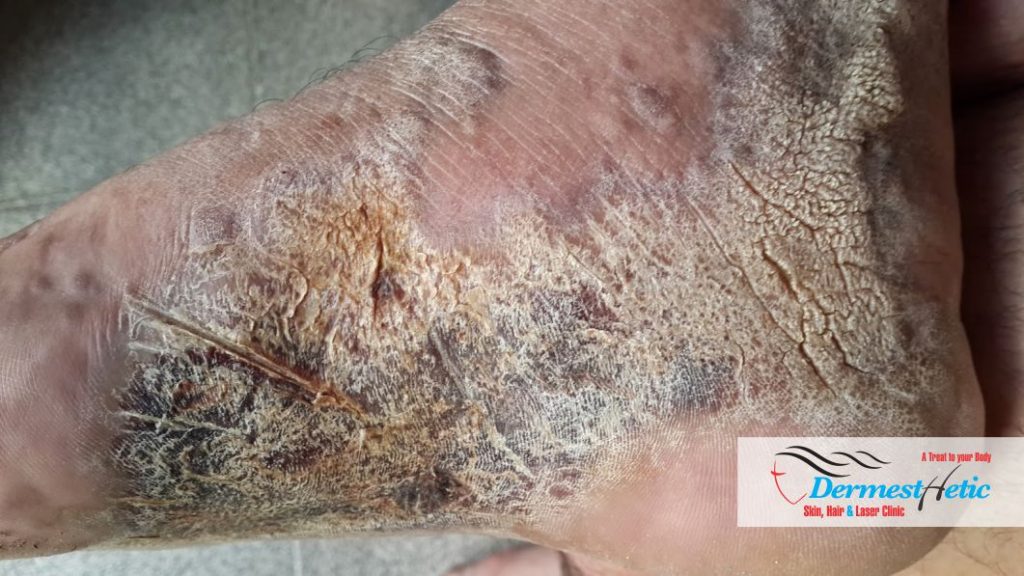
Generally, epidermal nevi on the head and face are more likely to be associated with malformations of the brain, eyes and cranial bones. Epidermal nevi on the trunk are more likely to be associated with abnormal curvature of the spine, hip malformation and deformities of the arms and legs. The lesions, apart from their appearance, usually do not cause additional symptoms. Individuals with a sebaceous nevus of the head may later develop intralesional tumors such as trichoblastoma or basal cell carcinoma. Recent research, however, suggests that this risk may be overstated in the medical literature. In fact, the risk of life-threatening malignant growth is virtually absent. Hence, there is no need to remove a sebaceous nevus for cancer prophylaxis.
We at DERMESTHETIC at Sialkot & Lahore, Pakistan have highly qualified Dermatologists/Cosmetologists who are expert in Epidermal Nevus Syndrome (ENS) treatments and procedures. And don’t forget, waiting for psoriasis to clear on its own can be frustrating. Without treatment, ENS can cause low self-esteem, depression and anxiety. To avoid these possible outcomes, dermatologists recommend that people treat ENS at an earliest stage as treatment may prevent new breakouts.
Types of Epidermal Nevus Syndrome (ENS)
We at DERMESTHETIC at Sialkot, Lahore, Pakistan have experienced dermatologists and cosmetologists treating the ENS along with counselling on psychological issue which may crop up due to ENS and properly advise the patients regarding the treatment.
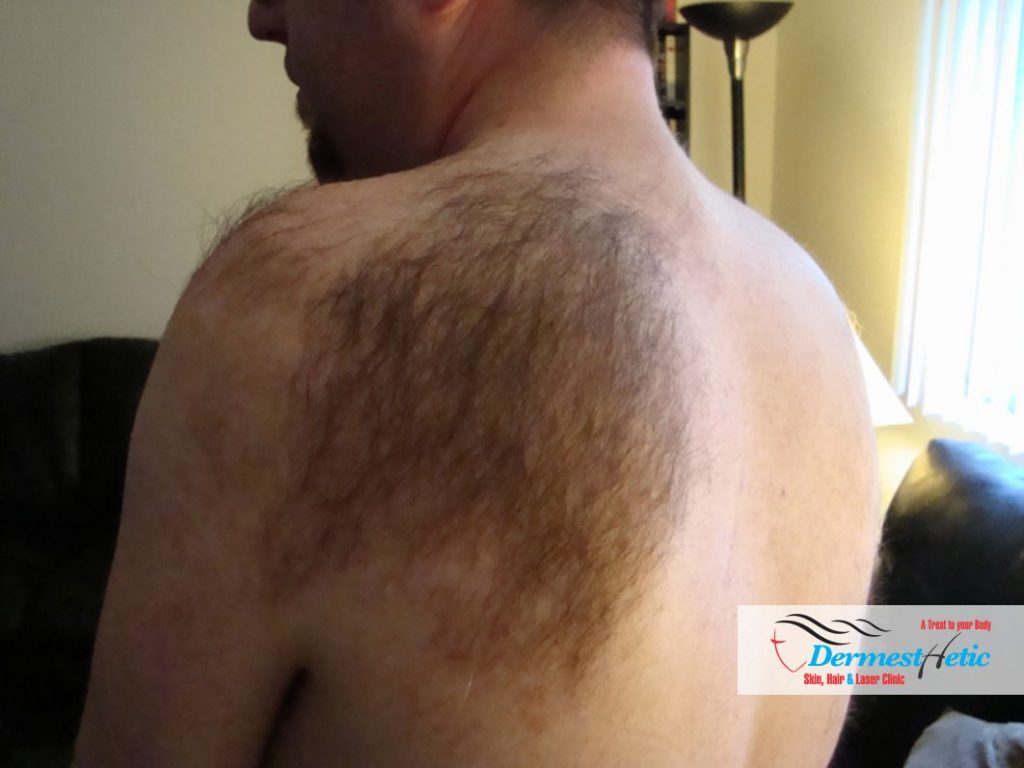
Types of ENS include:
- SCHIMMELPENNING SYNDROME (also known as sebaceous nevus syndrome) This disorder is characterized by multiple sebaceous nevi and defects affecting the brain, eyes and bones. The skin lesion affecting individuals with Schimmelpenning syndrome is called sebaceous nevus because it predominantly affects the sebaceous glands (small oil-producing glands in the skin). Schimmelpenning syndrome is the most common type of ENS. Sebaceous nevi are usually salmon or yellowed colored, hairless, smooth patches.
- PHACOMATOSIS PIGMENTOKERATOTICA, This type of ENS is characterized by the presence of a sebaceous nevus and a condition known as speckled lentiginous nevus of the papular type. Speckled lentiginous nevus is characterized by large, light-brown discoloration of the skin, superimposed by multiple darkened (melanocytic) spots (papules). While sebaceous nevus is present at birth, the characteristic papules of speckled lentiginous nevus may not develop until later in life, whereas the café-au-lait background macules showing a checkerboard arrangement tend likewise to be present in the newborn. Individuals with phacomatosis pigmentokeratotica may also develop additional abnormalities, especially neurological and skeletal abnormalities.
- NEVUS COMEDONICUS SYNDROME is characterized by numerous small, scaly, red or pink, droplet-like lesions (papules). These numerous spots of psoriasis appear over large areas of the body, primarily the trunk, but also the limbs and scalp. Guttate psoriasis is often triggered by a streptococcal infection, typically streptococcal pharyngitis. Guttate psoriasis is often starts in childhood or young adulthood, causes small, red spots, mainly on the torso and limbs. Triggers may be respiratory infections, strep throat, tonsillitis, stress, injury to the skin, and taking antimalarial and beta-blocker medications.
- NEVUS COMEDONICUS SYNDROME Nevus comedonicus is a skin lesion composed of closely-set, widened follicular openings that, in principle, belong to a hair follicle but in nevus comedonicus are plugged with keratin, a major structural protein found in the outer layer of skin as well as hair and nails. These lesions are often found on the head, but can also occur on the trunk and limbs. These lesions may be complicated by large cysts containing sebum (oil). Neurological abnormalities may also occur such as cognitive deficiencies, abnormal formation of the area of the brain that connects the two cerebral hemispheres (dysgenesis of the corpus callosum), and microcephaly, a condition that indicates that head circumference is smaller than would be expected for an infant’s age and gender.
- ANGORA HAIR NEVUS SYNDROME (SCHAUDER SYNDROME), is also known as Schauder syndrome. This type of ENS is characterized by an epidermal nevus that is covered by long, soft white hairs. The lesion is arranged in a broad, band-like shape. Angora hair nevus syndrome may be associated with seizures, intellectual impairment, and paralysis of one side of the body (hemiparesis).
- BECKER NEVUS SYNDROME may also be known as pigmented hairy epidermal nevus syndrome. A Becker nevus is characterized by one or more lesions that usually form a checkerboard pattern. A Becker nevus is characterized by over activity of hair follicles and pigment cells (melanocytes). Affected individuals have a large dark brown patch of skin that has often been reported to involve the shoulder, back or chest. However, this skin lesion can develop anywhere on the body. After puberty, a Becker nevus will darken and in males will show excessive hair growth. Some males with a Becker nevus may exhibit asymmetric growth of the beard.
- PROTEUS SYNDROME OR KERATINOCYTIC NEVUS SYNDROME A keratinocytic nevus is a linear skin lesion characterized by an overgrowth of keratinocytes, the predominant cell type in the epidermis. The characteristic finding of Proteus syndrome is overgrowth of various tissues of the body. The cause of the disorder is unknown. Disproportionate, asymmetric overgrowth occurs in a mosaic pattern (i.e., a random “patchy” pattern of affected and unaffected areas). Affected individuals may experience a wide variety of complications that may include progressive skeletal malformations, benign and malignant tumors, malformations of blood vessels (vascular malformations), bullous pulmonary disease, and certain skin lesions such as keratinocytic nevi. In some cases, life-threatening conditions relating to abnormal blood clotting may develop including deep vein thrombosis and pulmonary embolism.
- TYPE 2 SEGMENTAL COWDEN DISEASE Cowden disease is part of a group of disorders known as PTEN hamartoma syndromes, a spectrum of disorders caused by mutations of the PTEN gene. These disorders are characterized by multiple hamartomas that can affect various areas of the body. Type 2 segmental Cowden disease refers to a multisystem disorder caused by mutations of the PTEN gene that is also associated with a linear Cowden nevus, a type of keratinocytic nevus. Type 2 segmental Cowden disease is similar to Proteus syndrome and some cases have been misdiagnosed as Proteus syndrome.
- CHILD SYNDROME CHILD is an acronym for Congenital Hemidysplasia with Ichthyosiform nevus and Limb Defects. The disorder almost exclusively affects women and is present at birth. Symptoms generally affect one side of the body (hemidysplasia); the right side is affected twice as often as the left. Skin abnormalities present as inflamed reddish patches that are covered by large, waxy, yellowish scales. A wide variety of additional findings may occur on the same side of the body as the skin lesions including skeletal, neurological and visceral abnormalities.
- GARCIA-HAFNER-HAPPLE SYNDROME This form of ENS is characterized by a keratinocytic epidermal nevus that is soft and velvety in texture. Neurological abnormalities including seizures, intellectual impairment, degeneration of brain cells (cortical atrophy) and underdevelopment of the area of the brain that connects the two cerebral hemispheres (corpus callosum) can also occur. Skeletal abnormalities have not been reported in this disorder. Garcia-Hafner-Happle syndrome has only been reported in a handful of cases. It is caused by mutations to the fibroblast growth factor receptor 3 (FGFR) gene and is also called FGFR3 epidermal nevus syndrome.
- CLOVE SYNDROME an acronym for Congenital Lipomatous Overgrowth, Vascular malformations, and Epidermal nevus. CLOVE syndrome is extremely similar to Proteus syndrome and many individuals with this disorder were originally diagnosed with Proteus syndrome. According to the medical literature, the key difference is that overgrowth of toes in CLOVE syndrome is “ballooning”, nonprogressive and proportionate while with Proteus syndrome such overgrowth is distorted, progressive and disproportionate.
- NEVUS TRICHILEMMOCYSTICUS SYNDROME is haracterized by multiple cysts, which are derived from the root sheath of the hair follicle (trichilemmal cysts), that occur along with bone lesions.
- DIDYMOSIS APLASTICOSEBACEA the coexistence of a nevus sebaceous along with aplasia cutis congenita, a condition characterized by a lack of skin and hair in certain areas (localized), most often on the scalp. These lesions are usually localized and found close together.
- SCALP SYNDROME an acronym for Sebaceous nevus, Central nervous system malformations, Aplasia cutis congenital, Limbal Dermoid and Pigmented nevus.
- GOBELLO SYNDROME Gobello syndrome was associated with an organoid nevus with a velvety surface as well as excessive hairiness (hypertrichosis) and rough, elevated papules (follicular hyperkeratosis). Skeletal abnormalities were also present.
- BAEFVERSTEDT SYNDROME Baefverstedt syndrome was associated with abnormal horny growths on the skin in a linear pattern. Neurological symptoms such as intellectual disability and seizures were also noted. The horny growths developed on the face, neck and underarms and became quite prominent.
- NEVADA SYNDROME an acronym for Nevus Epidermicus Verrucosus with Angio Dysplasia and Aneurysms.
Treatment
We at DERMESTHETIC at Silakot & Lahore, Pakistan have experienced dermatologists and cosmetologists treating the Epidermal Nevus Syndrome (ENS) and properly advise the patient regarding the treatment after making proper diagnosis.
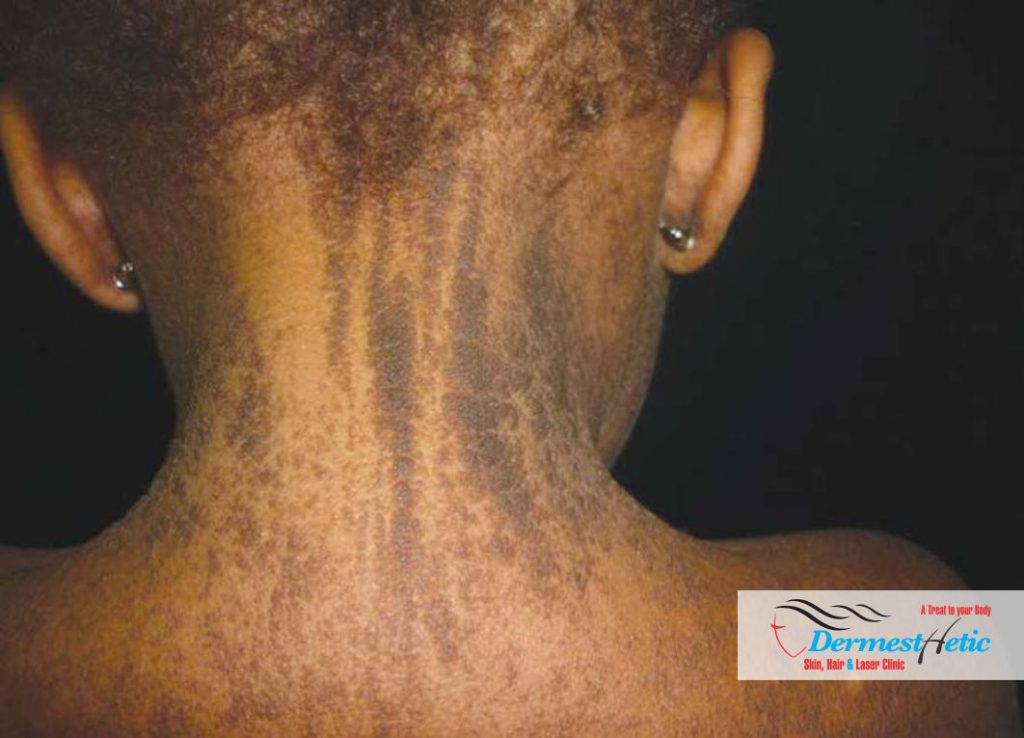
The treatment of ENS is directed toward the specific symptoms that are apparent in each individual. Treatment may require the coordinated efforts of a team of specialists. Pediatricians, pediatric neurologists, dermatologists, orthopedists, orthopedic surgeons, ophthalmologists and other healthcare professionals may need to systematically and comprehensively plan an affected treatment. Surgery may be performed to improve cosmetic appearance. However, surgical excision of a lesion may not always be possible due to the specific location of an epidermal nevus.
The specific therapeutic procedures and interventions for individuals with an ENS will vary, depending upon numerous factors including the specific symptoms present, the extent of the disorder, an individual’s age and overall health, tolerance of certain medications or procedures, personal preference and other factors. Decisions concerning the use of particular therapeutic interventions should be made by physicians and other members of the healthcare team in careful consultation with the patient and/or parents based upon the specifics of his or her case; a thorough discussion of the potential benefits and risks, including possible side effects and long-term effects; patient preference; and other appropriate factors.
Additional therapies that may be used to treat individuals with ENSs include remedial education, physical therapy and occupational therapy all of which should be individualized. Genetic counseling may be of benefit for affected individuals and their families. Other treatment is symptomatic and supportive. In the medical literature, several cases have been reported where neurosurgery has been used to treat individuals with an ENS and epilepsy.
Side Effects
These medicines have possible side effects, so patients must be carefully monitored. A possible serious side effect of using of a topical corticosteroid for a year or longer is skin atrophy. This means the skin becomes paper thin, very dry, and fragile. External “triggers” like medication, injury, phototherapy may start a new bout of psoriasis. These triggers aren’t the same for everyone. They may also change over time for you. The change in appearance caused by psoriasis can affect a person’s emotional and psychological well-being. People can experience emotional stress, particularly if psoriasis develops on visible areas of the body, such as the face, hands, or arms.