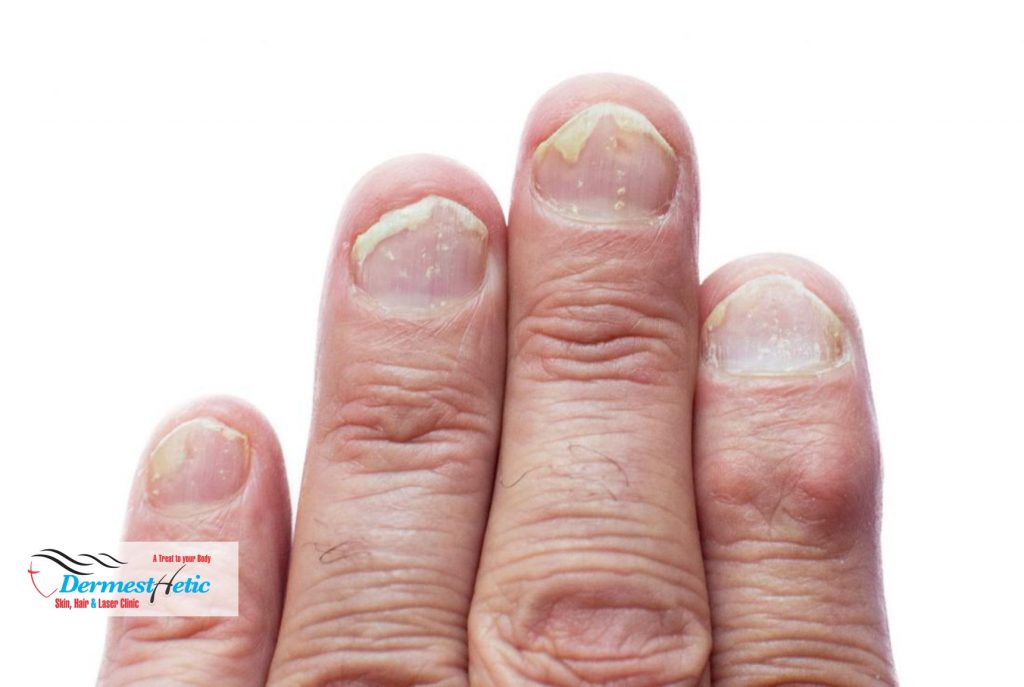
Psoriasis is a common skin condition that speeds up the life cycle of skin cells. It causes cells to build up rapidly on the surface of the skin. The extra skin cells form scales and red patches that are itchy and sometimes painful. Psoriasis is a long-lasting autoimmune disease characterized by patches of abnormal skin. These skin patches are typically red, dry, itchy, and scaly. On people with darker skin the patches may be purple in colour. Psoriasis varies in severity from small, localized patches to complete body coverage. Psoriasis is associated with other serious health conditions, such as diabetes, heart disease and depression.
Psoriasis is a chronic disease that often comes and goes. The main goal of treatment is to stop the skin cells from growing so quickly. They can grow anywhere, but most appear on the scalp, elbows, knees, and lower back. Psoriasis can’t be passed from person to person. It does sometimes happen in members of the same family. Psoriasis usually appears in early adulthood mostly affected persons of 20-30 years age and then another peak comes at 50-60 years of age for most patients. For most people, it affects just a few areas. In severe cases, psoriasis can cover large parts of the body. The patches can heal and then come back throughout a person’s life. If you develop a rash that doesn’t go away with an over-the-counter (OTC) medication, you should consider contacting your doctor. We at DERMESTHETIC Silakot & Lahore, Pakistan have experienced dermatologists and cosmetologists diagnosing and curing these diseases.
Conclusion
At DERMESTHETIC Silakot & Lahore, Pakistan we are committed to providing patients with the most advanced and authentic treatment of Psoriasis in Pakistan. In order to educate our patients in great detail about psoriasis in general, it’s causes, it’s different types of psoriasis and various treatment options available in the world, we provide a detailed information in this portion that the patients can educate themselves in befitting manner regarding their disease. The type of treatment that is best for you will depend on your preference, overall health, age, and where the psoriasis appears on your body. Some people choose not to treat psoriasis. It is not possible to predict how a patient will respond to treatment. It is important to keep in mind that no one treatment works for everyone. Results can vary from one part of the body to another. Psoriasis can be mild, moderate or severe. Your treatment options may depend on how severe your psoriasis is. Severity is based on how much of your body is affected by psoriasis.
If the symptoms are unclear or if your doctor wants to confirm their suspected diagnosis, they may take a small sample of skin. This is known as a biopsy. The skin will be sent to a lab, where it’ll be examined under a microscope. The examination can diagnose the type of psoriasis you have. It can also rule out other possible disorders or infections. The entire hand (the palm, fingers and thumb) is equal to about 1 percent of your body surface area. Combining two or more treatments often gives the best results. Before starting treatment, a dermatologist should be consulted. We at DERMESTHETIC have such expertise and knowledge and you may meet with our doctors who are rated as the BEST SKIN SPECIALISTS AND DERMATOLOGISTS IN LAHORE, PAKISTAN with special interest in psoriasis.
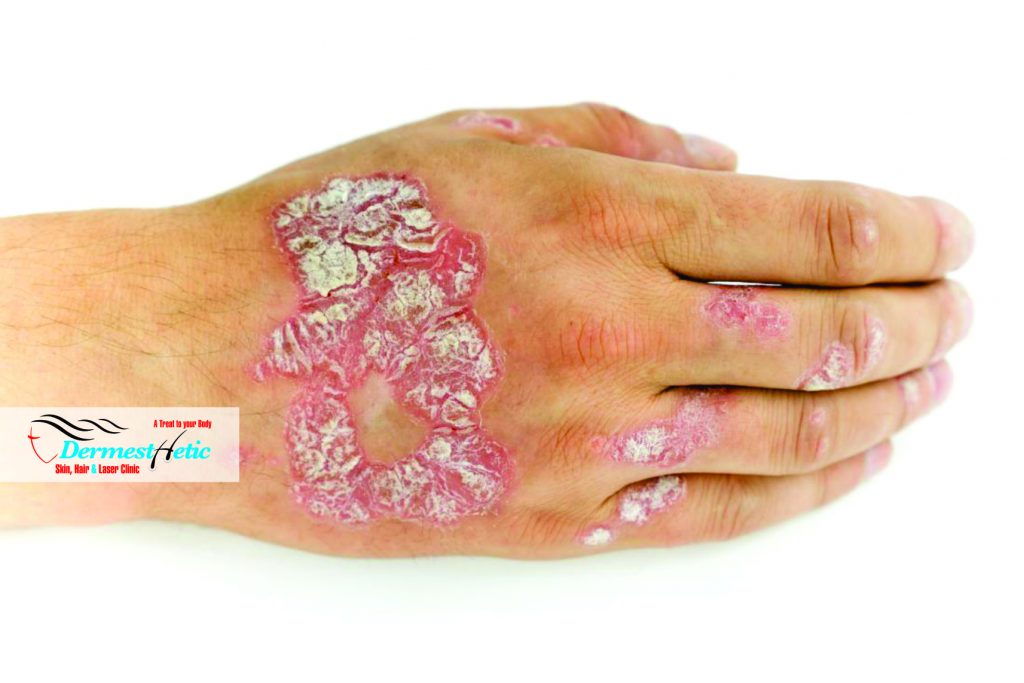
Causes
The cause of psoriasis isn’t fully understood, but it’s thought to be related to an immune system problem with T cells and other white blood cells, called neutrophils, in your body. While scientists do not know what exactly causes psoriasis, we do know that the immune system and genetics play major roles in its development. Usually, something triggers psoriasis to flare. The skin cells in people with psoriasis grow at an abnormally fast rate, which causes the buildup of psoriasis lesions. Men and women develop psoriasis at equal rates. Psoriasis also occurs in all racial groups, but at varying rates. Psoriasis is not contagious. It is not something you can “catch” or that others can catch from you. Psoriasis lesions are not infectious. Researchers think something sets off your immune system. The exact reason is a mystery. But it’s likely a combination of genetics and triggers.
- Genes and Immune System: When you have psoriasis, the genes that control your immune system signals get mixed up. Instead of protecting your body from invaders as it’s designed to do, it promotes inflammation and turns skin cells on overdrive.
- Hormone Changes: The disease often shows up or flares during puberty. Menopause can also trigger it. During pregnancy, your symptoms may get better or even go away. But after the baby’s born, you might have a flare.
- Smoking/Alcohol: Lighting up can double your risk of getting psoriasis. It’s closely linked with a hard-to-treat type called pustular psoriasis, which affects the palms of your hands and the soles of your feet. Heavy drinkers have a higher risk, especially younger men. Alcohol can make treatments less effective, too.
- Stress: Scientists think your immune system may respond to emotional and mental pressures the same way it does to physical problems like injuries and infections.
- Medications: Some treatments can make psoriasis worse. These include:
Lithium which treats bipolar disorder and other mental illnesses, High blood pressure and heart medicines, including propranolol (Inderal) and other beta-blockers, ACE inhibitors, and quinidine, Antimalarial medicines, including chloroquine, hydroxychloroquine (Plaquenil) and quinacrine, Indomethacin (Indocin), which treats inflammation.
- HIV: Psoriasis usually is worse in the beginning stages of HIV infection, but then it gets better after you start certain treatments.
- Other Infections: Strep infections, in particular, are linked with guttate psoriasis, which looks like small, red drops. Kids will often have strep throat before their first flare. Earaches, bronchitis, tonsillitis, or a respiratory infection such as a cold, the flu, or skin problems.
- Sunlight: A little natural sunlight is good for most people with psoriasis. But for a few, the sun makes their condition worse. So can a bad sunburn, so protect your skin if you’re going to be outside.
- Skin Injuries: A cut, scrape, bug bite, infection, or too much scratching can trigger the condition.
- Weight: People who are obese tend to get plaques in their skin creases and folds.
- Weather: Your psoriasis might be worse in the winter. Dry air, less natural sunlight, and cold temperatures can make symptoms worse. Keep your skin moist, and try a humidifier at home.
Symptoms
Cells normally travel through the body to defend against foreign substances, such as viruses or bacteria. But if you have psoriasis, the cells attack healthy skin cells by mistake, as if to heal a wound or to fight an infection. Overactive cells also trigger increased production of healthy skin cells, more T cells and other white blood cells, especially neutrophils. These travel into the skin causing redness and sometimes pus in pustular lesions. Dilated blood vessels in psoriasis-affected areas create warmth and redness in the skin lesions. The process becomes an ongoing cycle in which new skin cells move to the outermost layer of skin too quickly in days rather than weeks. Skin cells build up in thick, scaly patches on the skin’s surface, continuing until treatment stops the cycle.
What causes cells to malfunction in people with psoriasis isn’t entirely clear. Researchers believe both genetics and environmental factors play a role. Psoriasis signs and symptoms are different for everyone. Common signs and symptoms include:
- Red patches of skin covered with thick, silvery scales
- Small scaling spots (commonly seen in children)
- Dry, cracked skin that may bleed
- Itching, burning or soreness
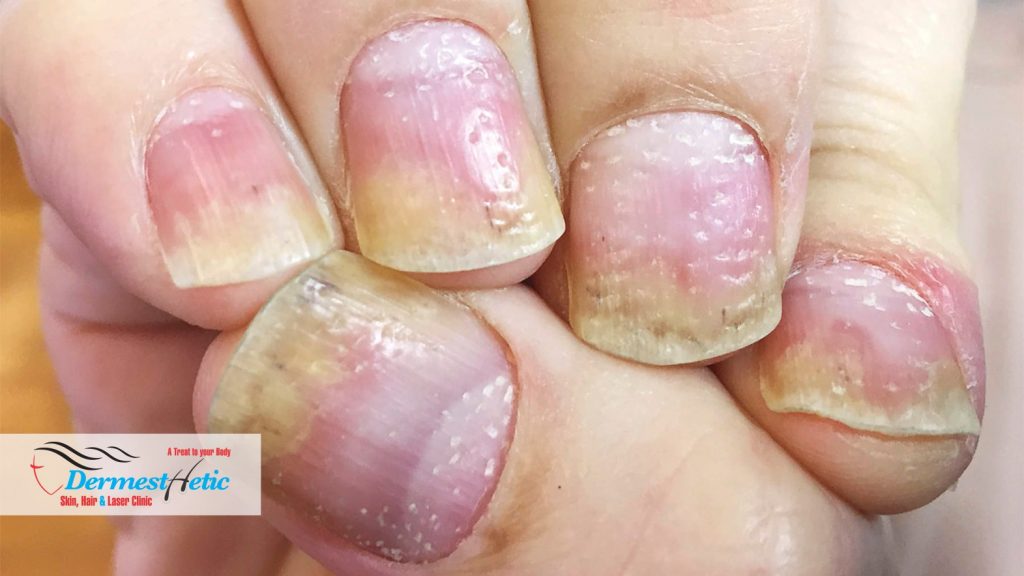
- Thickened, pitted or ridged nails
- Swollen and stiff joints
Psoriasis patches can range from a few spots of dandruff-like scaling to major eruptions that cover large area. Most types of psoriasis go through cycles, flaring for a few weeks or months, then subsiding for a time or even going into complete remission.
We at DERMESTHETIC at Silakot & Lahore, Pakistan have highly qualified Dermatologists/Cosmetologists who are expert in psoriasis treatments and procedures. And don’t forget, waiting for psoriasis to clear on its own can be frustrating. Without treatment, psoriasis can cause low self-esteem, depression and anxiety. To avoid these possible outcomes, dermatologists recommend that people treat psoriasis at an earliest stage as treatment may prevent new breakouts.
Types of Psoriasis
We at DERMESTHETIC at Sialkot, Lahore, Pakistan have experienced dermatologists and cosmetologists treating the psoriasis along with counselling on psychological issue which may crop up due to psoriasis and properly advise the patients regarding the treatment.
Types of psoriasis include:
- Plaque psoriasis or Psoriasis vulgaris (also known as chronic stationary psoriasis or plaque-like psoriasis) is the most common form. Plaque psoriasis causes dry, raised, red skin lesions (plaques) covered with silvery scales. The plaques might be itchy or painful and there may be few or many. They can occur anywhere on your body, including your genitals and the soft tissue inside your mouth. Plaque psoriasis typically appears as raised areas of inflamed skin covered with silvery-white scaly skin. These areas are called plaques and are most commonly found on the elbows, knees, scalp, and back.
- Pustular psoriasis, which causes red and scaly skin with tiny pustules on the palms of the hands and soles of the feet. Pustular psoriasis appears as raised bumps filled with noninfectious pus (pustules). The skin under and surrounding the pustules is red and tender.
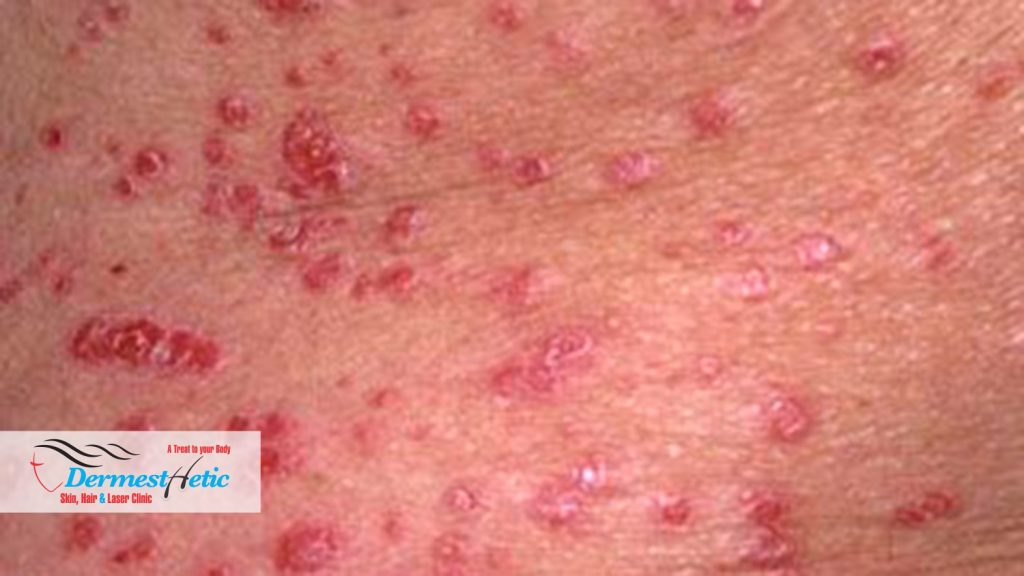
- Guttate psoriasis is characterized by numerous small, scaly, red or pink, droplet-like lesions (papules). These numerous spots of psoriasis appear over large areas of the body, primarily the trunk, but also the limbs and scalp. Guttate psoriasis is often triggered by a streptococcal infection, typically streptococcal pharyngitis. Guttate psoriasis is often starts in childhood or young adulthood, causes small, red spots, mainly on the torso and limbs. Triggers may be respiratory infections, strep throat, tonsillitis, stress, injury to the skin, and taking antimalarial and beta-blocker medications.
- Inverse psoriasis (also known as flexural psoriasis) appears as smooth, inflamed patches of skin. The patches frequently affect skin folds, particularly around the genitals (between the thigh and groin), the armpits, in the skin folds of an overweight abdomen (known as panniculus), between the buttocks in the intergluteal cleft, and under the breasts in the inframammary fold. Heat, trauma, and infection are thought to play a role in the development of this atypical form of psoriasis.
- Erythrodermic psoriasis, or Psoriatic erythroderma involves widespread inflammation and exfoliation of the skin over most of the body surface. It may be accompanied by severe dryness, itching, swelling, and pain. It is often the result of an exacerbation of unstable plaque psoriasis, particularly following the abrupt withdrawal of systemic glucocorticoids. This form of psoriasis can be fatal as the extreme inflammation and exfoliation disrupt the body’s ability to regulate temperature and perform barrier functions. Erythrodermic psoriasis which causes fiery redness of the skin and shedding of scales in sheets. It’s triggered by severe sunburn, infections, certain medications, and stopping some kinds of psoriasis treatment. It needs to be treated immediately because it can lead to severe illness.
- Nail psoriasis can affect fingernails and toenails, causing pitting, abnormal nail growth and discoloration. Psoriasis can affect the nails and produces a variety of changes in the appearance of finger and toe nails. These changes include pitting of the nails (pinhead-sized depressions in the nail is seen in 70% with nail psoriasis), whitening of the nail, small areas of bleeding from capillaries under the nail, yellow-reddish discoloration of the nails known as the oil drop or salmon spot, dryness, thickening of the skin under the nail (subungual hyperkeratosis), loosening and separation of the nail (onycholysis), and crumbling of the nail Psoriatic nails might loosen and separate from the nail bed (onycholysis). Severe cases may cause the nail to crumble.
- Seborrheic-like psoriasis is a common form of psoriasis with clinical aspects of psoriasis and seborrheic dermatitis and it may be difficult to distinguish from the latter. This form of psoriasis typically manifests as red plaques with greasy scales in areas of higher sebum production such as the scalp, forehead, skin folds next to the nose, skin surrounding the mouth, skin on the chest above the sternum and in skin folds.
- Psoriatic arthritis is a form of chronic inflammatory arthritis that has a highly variable clinical presentation and frequently occurs in association with skin and nail psoriasis. It typically involves painful inflammation of the joints and surrounding connective tissue and can occur in any joint, but most commonly affects the joints of the fingers and toes. This can result in a sausage-shaped swelling of the fingers and toes known as dactylitis. Psoriatic arthritis can also affect the hips, knees, spine (spondylitis) and sacroiliac joint(sacroiliitis). In addition to inflamed, scaly skin, psoriatic arthritis causes swollen, painful joints that are typical of arthritis. Sometimes the joint symptoms are the first or only manifestation of psoriasis or at times only nail changes are seen.
- Napkin psoriasis is a subtype of psoriasis common in infants characterized by red papules with silver scale in the diaper area that may extend to the torso or limbs. Napkin psoriasis is often misdiagnosed as napkin dermatitis or diaper rash.
Treatments
We at DERMESTHETIC at Silakot & Lahore, Pakistan have experienced dermatologists and cosmetologists treating the vitiligo and properly advise the patient regarding the treatment after making proper diagnosis.
There is no cure for psoriasis; however, various treatments can help control the symptoms. These treatments include steroid creams, vitamin D3 cream, ultraviolet light and immune system suppressing medications, such as methotrexate. About 75 percent of cases can be managed with creams alone. The disease affects two to four percent of the population. Men and women are affected with equal frequency. The disease may begin at any age, but typically starts in adulthood. Psoriasis is associated with an increased risk of psoriatic arthritis, lymphomas, cardiovascular disease, Crohn’s disease and depression. Psoriatic arthritis affects up to 30 percent of individuals with psoriasis.
The most common types of therapies/medicines that doctors use to treat vitiligo include:
- Immune mediators: Topical preparations of immune suppressing medications including glucocorticoids (such as 0.05% clobetasol or 0.10% betamethasone) and calcineurin inhibitors (such as tacrolimus or pimecrolimus) are considered to be first-line vitiligo treatments.
- Phototherapy: Phototherapy is considered a second-line treatment for vitiligo. Exposing the skin to light from UVB lamps is the most common treatment for vitiligo. The treatments can be done at home with an UVB lamp or in a clinic. The exposure time is managed so that the skin does not suffer overexposure. Treatment can take a few weeks if the spots are on the neck and face and if they existed not more than 3 years.
- PUVA light therapy: Uses UVA light and a medicine called psoralen to restore skin color. Psoralen may be applied to the skin or taken as a pill. Psoralen can affect the eyes, so this treatment requires an eye exam before and after finishing treatment.
- Vitamins, minerals etc: Some vitamins, minerals, amino acids, and enzymes have been reported to restore skin color in people who have vitiligo. Ginkgo biloba, an herb, has been studied in a clinical trial. Results from this trial indicate that the herb may restore skin color and stop vitiligo from worsening.
- Creams, Sunblocks: The treatment usually consists of medicated creams, treatment with ultraviolet light in your dermatologist’s clinic, and sometimes oral medications with ultraviolet light.
- Skin Camouflage: In mild cases, vitiligo patches can be hidden with makeup or other cosmetic camouflage solutions. If the affected person is pale-skinned, the patches can be made less visible by avoiding tanning of unaffected skin.
- Di-pigmenting: In cases of extensive vitiligo the option to de-pigment the unaffected skin with topical drugs like monobenzone, mequinol, or hydroquinone may be considered to render the skin an even colour. The removal of all the skin pigment with monobenzone is permanent and vigorous. Sun-safety must be adhered to for life to avoid severe sunburn and melanomas. Depigmentation takes about a year to complete.
- Surgery: May be an option when light therapy and medicines applied to the skin do not work. Different surgical procedures are available. Most involve removing skin with your natural color or skin cells and placing these where you need color.
- Melanocyte Transplant: In this treatment the color producing cells are transferred from the normal skin to the white spots, where they start producing the skin color. Several transplantation techniques have been developed, including transplantation of melanocyte precursors derived from hair follicles. Transplantation procedures are frequently used to treat segmental vitiligo which is poorly responsive to other types of treatment.
Side Effects
These medicines have possible side effects, so patients must be carefully monitored. A possible serious side effect of using of a topical corticosteroid for a year or longer is skin atrophy. This means the skin becomes paper thin, very dry, and fragile. External “triggers” like medication, injury, phototherapy may start a new bout of psoriasis. These triggers aren’t the same for everyone. They may also change over time for you. The change in appearance caused by psoriasis can affect a person’s emotional and psychological well-being. People can experience emotional stress, particularly if psoriasis develops on visible areas of the body, such as the face, hands, or arms.